Negotiating the pharmaceutical roller coaster
I have been noticing that there is a ‘creep’ phenomenon happening in regards to medical drug use as we age.
One drug may lead to the next. Often this is to offset the side effects of a certain medication and this in turn may trigger further, different disease states. This is termed ‘Polypharmacy’. This is dangerous as your body is put under further strain to minimise the damaging effects of combinations of medications.
Why do we buy into the medication cycle?
As we get older more health issues may arise, and we become more aware of – and fearful of – death and dying and ageing. We keep hearing about our friends and well-known age peers having health crises – heart attacks, strokes, diabetes, cancer – and this makes it feel closer to home – it’s scary.
Most of us trust the advice of our GP unquestioningly – because that’s what we’ve been taught all our lives. However, ageing is a natural process, not a disease.
It’s also a process that the global pharmaceutical industry has targeted as a major market growth opportunity as the baby boomer generation moves into retirement.
Disease care is not HEALTH care
Here’s one story from my practice:
A 65 year old man Jason (not his real name) was given Blood Pressure medication at a crisis time in his life. He was severely stressed from multiple sources – going through retirement, money stress and relationship issues.
He kept taking the medication over the next 2 years with random doctor’s appointments to measure BP etc. But there was never any question of reducing or stopping the medication.
Jason’s doctor’s expectation is for him to be on it ‘for life’. Why? Because the doctor considered it “too hard” to attend to lifestyle issues that are pervasive in our industrialised, sedentary society.
It was easier to repeat the script month in, month out for decades. This attitude is absorbed automatically by the patient – he wanted to be a ‘good patient’ and not upset the apple cart or “waste time” by asking questions and exploring his options.
So a medication Jason started in a time of stress became permanent.
What’s the problem with blood pressure medication anyway? Long term use can contribute to kidney damage especially when other medications like NSAIDS are added to the mix. Short term side effects may be: cough, diarrhoea, constipation, dizziness (predispose you to falls), erection problems, feeling nervous or tired, headache, nausea or vomiting.
Taking time to discuss options with 65 year old Jason gave him a fresh perspective and ideas to take charge of this potential roller coaster. He decided to join a men’s walking group and the local Rotary Club where he felt he could contribute some of his life experience in business to support others. He opted to use some herbal medications and made some dietary adjustments I recommended while still taking his Blood Pressure meds and agreed to regular follow up consults with his GP and with me.
Jason understands this is a slow gentle process as his being adjusts to greater wellness. Over time as his blood pressure is better managed he will wean off (with the help of his GP) the more aggressive medications as his lifestyle supports help balance his body/mind.
There are ways to take back control of the medication train
Doctors are trained to treat disease when it occurs – to treat your body like a mechanical machine doomed to wear out and break down over time. That approach makes sense for acute diseases like appendicitis or extreme acute pain – but a lot less sense for a natural process like ageing.
And taking multiple medications for multiple “conditions” multiplies the side effects and health risks.
So what do you do?



1. Take a whole-of-lifestyle approach
Tell your GP you’d like to explore lifestyle options and /or Naturopathic support for your condition. (If this is too confronting you can do plenty of lifestyle changes without changing your current medication or telling your GP. )
- Address your approach to exercise:
Work with someone to support you with a regular regime for your particular needs – a friend, partner, colleague, fitness instructor, gym coach, personal coach, Naturopath, osteopath, physiotherapist, chiropractor etc – Someone you trust and can confide in and has your best interests in their sights.
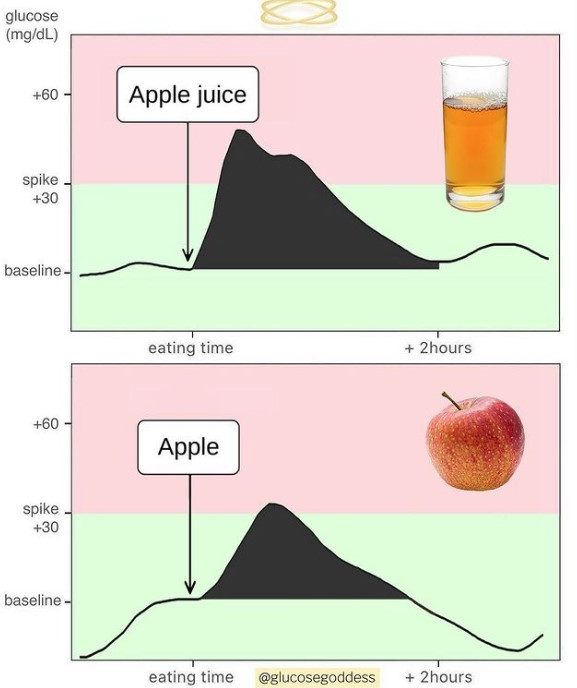
- Consider your daily food intake:
How much sugar do you eat, hidden or otherwise?
What is the quantity and quality of your food?
What are your habits surrounding food and fluid intake?
What variety of foods do you eat?
Monitor your appetite and joy of taste and sensation.
Keep a diary of your daily foods and fluids and your reactions to these. Chat to a Naturopath or Nutritionist about your individual needs.
- Monitor yourself
If you are using Blood pressure medication, find a reliable blood pressure monitor from your pharmacy and self monitor several times per week at different times of the day.
Keep a record to show a Practitioner later.
This can be empowering for your overall feeling of well-being.
If you take medication for gut issues, keep a diary of your food intake and gut responses and a range of other factors you feel may impact you – like emotions, menstrual timing, stressful events, exercise etc.
- Consider daily stress management
Trial strategies like meditation, walking, nature exposure, positive self talk, rest and relaxation, regular bodywork like massage etc. Even if you don’t ‘feel’ stressed, all the small micro stress challenges of a day add into the overall bucket of stress. This has an adverse cumulative effect unless we weave intentional relaxation manoeuvres into our daily routine. - Connecting in a meaningful way with other people has been shown to be essential for our well-being. Having one or two close friends in important. Research about micro stressors shows that it takes about 200 hours of person to person contact to establish a meaningful close relationship.
- Another important de-stressor is to be actively involved in at least 2 groups of people away from work or home activities. Consider a walking group, singing group, yoga group, tennis club, turtle rescue group etc.
2. Understand your medication
- Research the drugs you’re taking on the internet – using reputable sites like Pubmed and nps.org.au
NPS MedicineWise is a not-for-profit, unbiased, Australian based education portal for medicines sold here. - Know your meds.
Know the dose you take and when you should take it. Know any interactions with other medications or foods. Know how long is a ‘safe’ time frame to be on the medication. For example Protein Pump Inhibitors, like Somac, Omeprazole etc (to reduce reflux) are only designed to be taken for about 4 to 6 weeks. How many people do you know who have been on them for years?
You may think your GP will tell you all this, but they really don’t have the time to check everything for everybody. Use your pharmacist as a resource – they have a duty of care as well as your GP to keep you safe and help you understand your meds.
Ask about all the side effects, long and short term. Weigh up the risks for yourself. Ask about the research . You’ll be surprised how little research has been done especially in regards to interactions between numerous medications.
Ask your family or another health professional like a Naturopath to help research the medications if you are not comfortable understanding or researching the literature.
3. Discuss alternatives with your Naturopath
- Seek detailed guidance on suitable nutritional and/herbal medicine options that can be taken safely in conjunction with your current medication(s).
There are a whole range of centuries-old complementary medicines that are outside the medical knowledge base the pharmaceutical industry supplies to your GP. - Find lifestyle change support – invest in building habits and practices to support your health – such as a naturopath, nutritionist, counsellor, personal trainer, massage therapist, physiotherapist, acupuncturist or other health professional.